NFP’s Modern Marvels Draws Millennials, Scientists and Some Pushback, by Peter Jesserer Smith
Founder’s Quote
July 17, 2019
Parenthood Parenthood Fires CEO Leana Wen After 10 Months, Wants More Aggressive Pro-Abortion Leader, by Steven Ertelt
July 17, 2019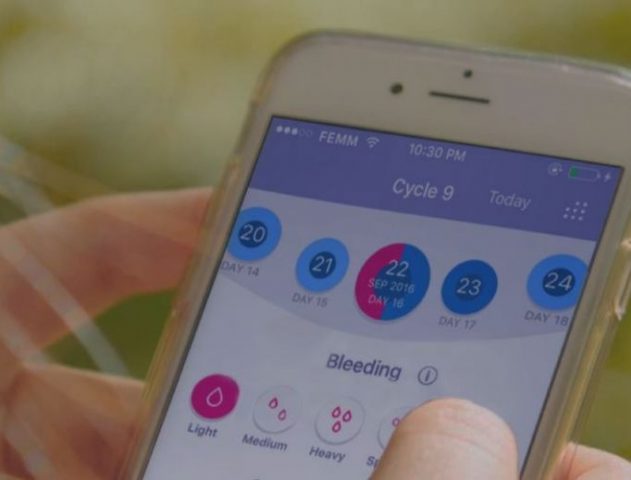
New apps are helping couples start their families, particularly millennials. Dr. Rachel Peragallo Urrutia, lead author of ‘Effectiveness of Fertility Awareness-Based Methods for Pregnancy Prevention: A Systematic Review,’ is shown below.
A recent salvo by The Guardian indicates that fertility-awareness-based methods are leaving their niche in Catholic circles and entering the mainstream.
More millennial women than ever are turning to fertility-awareness-based methods, not simply for a natural way to plan their families, but as a way to keep track of their bodily health and well-being without putting hormones or artificial devices into their bodies.
“I’m a millennial, and we’re just kind of tired of anything that looks like it’s from the 1970s, especially for our health,” Cassie Moriarity, a 29-year-old Catholic woman living in New York City, told the Register.
New digital technology has been transforming fertility-awareness-based methods, or FABMs, and empowering millennials like Moriarity to take charge of their health and fertility. It has also offered them natural family planning alternatives to artificial forms of birth control, such as the pill or intrauterine devices (IUDs).
Moriarity, a married mother of one child, said she began tracking her health through FABMs when she was 20, keeping charts through her favorite apps on her phone. After getting married, she used a variety of FABMs to conceive and then postpone pregnancy. Today, Moriarity uses the app-based FEMM (Fertility Education and Medical Management) Health system and is an instructor who teaches classes one-on-one or via Google Hangouts.
“What I really liked about FEMM was the model really simplified a lot of NFP material,” she said, explaining the method relies on one main fertility sign as a biomarker of women’s health and fertility.
Overall, FABMs and NFP are leaving the niche world of Catholic and Christian communities for the secular mainstream.
Because more millennials are adopting FABMs, particularly as forms of natural family planning (NFP), scientific researchers are giving them renewed scrutiny. Meanwhile, they are generating pushback from advocates of artificial birth control.
Alarmed that more than 400,000 people worldwide had downloaded the FEMM app, The Guardian newspaper launched a broadside against FEMM. The United Kingdom-based publication alleged FEMM had a hidden pro-life and anti-birth-control agenda and stated NFP methods had 23% failure rates to prevent pregnancy.
But The Guardian’s reporting came just as the Centers for Disease Control(CDC) released new data on NFP method rates. The CDC has now acknowledged, based on a 2018 systematic review published in the American Centers of Obstetrics and Gynecology (ACOG) journal, Obstetrics and Gynecology, that typical failure rates to prevent pregnancy in NFP actually range between 2% and 23%, depending on the method.
A University of Iowa study published in 2009 predicted that the obstacle to widespread adoption of FABMs was simply lack of information. While between 1% and 3% of women in the U.S. use fertility-awareness methods to postpone pregnancy, the study found that number could jump to 1 out of 5 women if they were informed about these methods.
“Knowledge is increasing, people are following this closely, and they’re looking for healthy alternatives,” Anna Halpine, CEO of FEMM Health, said. Halpine said FEMM has users all over the world, and its use is growing, particularly in Latin America and Africa. Many users are not wealthy, and at the FEMM-affiliated clinic in Columbus, Ohio, half of the users are Medicaid patients.
New NFP Methods Gaining Recognition
At present, most NFP methods using apps and technology in the U.S. are based on “off-label” uses of technology that is presently marketed as an aid to achieving pregnancy. But that is slowly starting to change, as funders start to line up behind medical researchers and developers of this technology that need data to convince the Food and Drug Administration to recognize them.
“Natural Cycles,” an app that is already recognized by the European Union as a tool that can be used to avoid pregnancy, has now received similar recognition by the FDA, making it the first FABM app or device to have permission in the U.S. to market itself as a way to avoid pregnancy.
Richard Fehring, director of Marquette University’s Institute for Natural Family Planning, told the Register that many millennials, who tend to be more conscious about the environment and what they put into their bodies, are looking for natural alternatives to artificial birth control for family planning and are driving the explosion of FABM apps.
He noted that not all millennials using these apps are engaged fully in natural family planning, which involves abstinence during the fertile period, as supported by Church teaching. Some add condoms during the fertile cycle, as determined by the FABM. But, he said, “it is a step in getting away from the pill.”
FEMM System
Moriarty explained a woman may need different FABMs depending on the needs of her body and life circumstances, or if it involves NFP, the needs of her spouse, as well. Her own life experience has reflected that.
Morarity said she likes FEMM’s “science and evidence-based model” for women looking to take care of their health and as a way to do NFP. The FEMM system, she said, simplified a lot of the interpretations of fertility signs over other FABMs she used and allowed her to track the data via app and discuss questions with an instructor.
Halpine explained many women have chosen FEMM and other FABMs because they are aware of the reported adverse health effects (or experienced them personally) from hormonal contraception or artificial devices. While many women use FEMM to help them achieve or postpone pregnancy, the main focus of FEMM is helping women care for their health.
Halpine described FEMM as “a comprehensive women’s health care system” that trains health educators and medical providers and works directly with women. App users can be linked to FEMM teachers to receive feedback and support about their health questions and fertility goals and be directed to affiliated clinics and health professionals who can help them with any problems that emerge.
“Fertility is certainly a very important application for many of our users, but we believe every woman should understand how her body works, what is healthy and normal at every stage of her life, and be able to reach out and get support when needed as that changes,” she said. “FEMM tries to provide that support and knowledge.”
Scientific Research
Marquette’s Fehring said that new technology is coming onto the scene, which, along with apps, is making NFP increasingly accurate, effective and affordable.
Fehring indicated the increased attention on FABMs will provide greater impetus for medical peer review to test claims about the effectiveness of different NFP systems, apps and technology.
He said the systematic review published by ACOG did a “tremendous amount of work,” which will help more doctors and scientists “develop secure, evidence-based studies” on FABMs and NFP and for physicians and other health professionals to consider recommending them for their patients.
Dr. Rachel Peragallo Urrutia, lead author of the ACOG-published review “Effectiveness of Fertility Awareness-Based Methods for Pregnancy Prevention: A Systematic Review,” told the Register that her team evaluated all the studies they could find on different fertility-based-awareness methods. She said they intended their study to provide a “baseline of all that is out there.” 
The paper reflects the consensus of a multidisciplinary team, with some members coming from a NFP and religious perspective and others from a contraceptive, family-planning, “pro-choice” perspective.
“We were able to agree on the important facts of the study,” she said, adding that it helped the credibility of the study to have this broad range of perspectives and to be published in a credible journal.
The review ranked studies of different FABMs into three categories: “high quality,” “moderate quality” and “low quality.” Urrutia explained that no FABM study met their “high quality” category and its 13 attainable criteria.
Many studies met the “moderate quality” category, which she said meant the researchers “could trust the data enough to report it and talk about it, but it’s not the highest level of data.”
More Data Needed
According to the ACOG review, the top two methods for effectiveness in avoiding pregnancy were the Marquette Method and Sensiplan. But until they have “high quality” studies, Urrutia said her team cannot conclusively say which FABM is the most effective at avoiding pregnancy.
Many FABM studies were found to be “low quality,” meaning “there was a significant enough concern that we could not trust the findings enough to report the estimates of those studies.”
Urrutia said many of these studies “didn’t do the appropriate statistical techniques” needed to prevent inflating the actual effectiveness rate of a particular FABM. She explained that a study on a FABM should calculate its effectiveness rate from the total number of pregnancies divided by the number of cycles for which the method was used correctly.
“But a lot of studies just put in the total number of cycles, not just where it was used correctly, and that makes it look better than it actually was,” she said.
Some other FABM studies Urrutia’s team reviewed also did not exclude women who were abstaining completely from sex during the cycle. Urrutia explained that finding out the “apples-to-apples” effectiveness of an FABM against artificial contraceptives for preventing pregnancy means the women in both cases have to be having sex and trying to avoid pregnancy in their cycles.
Some FABM effectiveness studies failed to ask women in advance if they wanted to get pregnant that cycle or how much they wanted to avoid pregnancy that cycle or provide follow-up. Other studies, such as the Creighton Model studies, tried to determine “after the fact” whether a woman intended to get pregnant or not.
Urrutia said all the present Creighton Model studies are “low quality,” but her colleague Dr. Joseph Stanford is conducting a Creighton Model study that aims to meet the “high quality” criteria.
Giving New Providers Confidence
Urrutia said she and her team hope this systematic review provides a baseline and “specific and very clear criteria” that will lead to the development of future “high quality” FABM studies and give health providers more options they can have confidence in.
“All of us agree women deserve accurate, transparent methods,” she said.
She said fully funded, medical peer-reviewed research can help clear up the “wild west of apps” and encourage newer methods and apps that want to set themselves apart from the competition “to actually publish data and not make claims they can’t support with data.”
She added, “The more studies we have, the more we can be sure that one method is really better than another.”
Peter Jesserer Smith is a Register staff writer.




